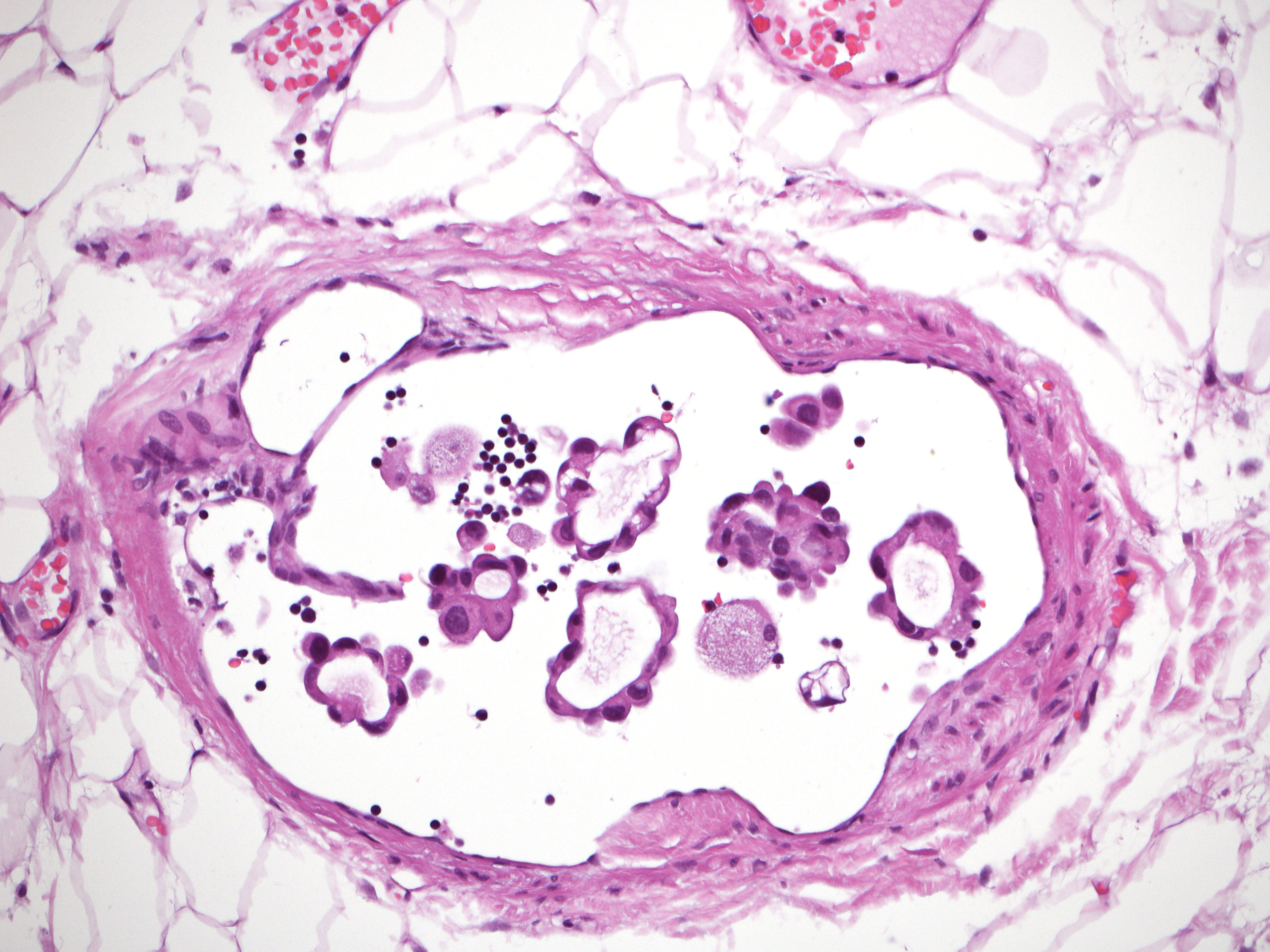
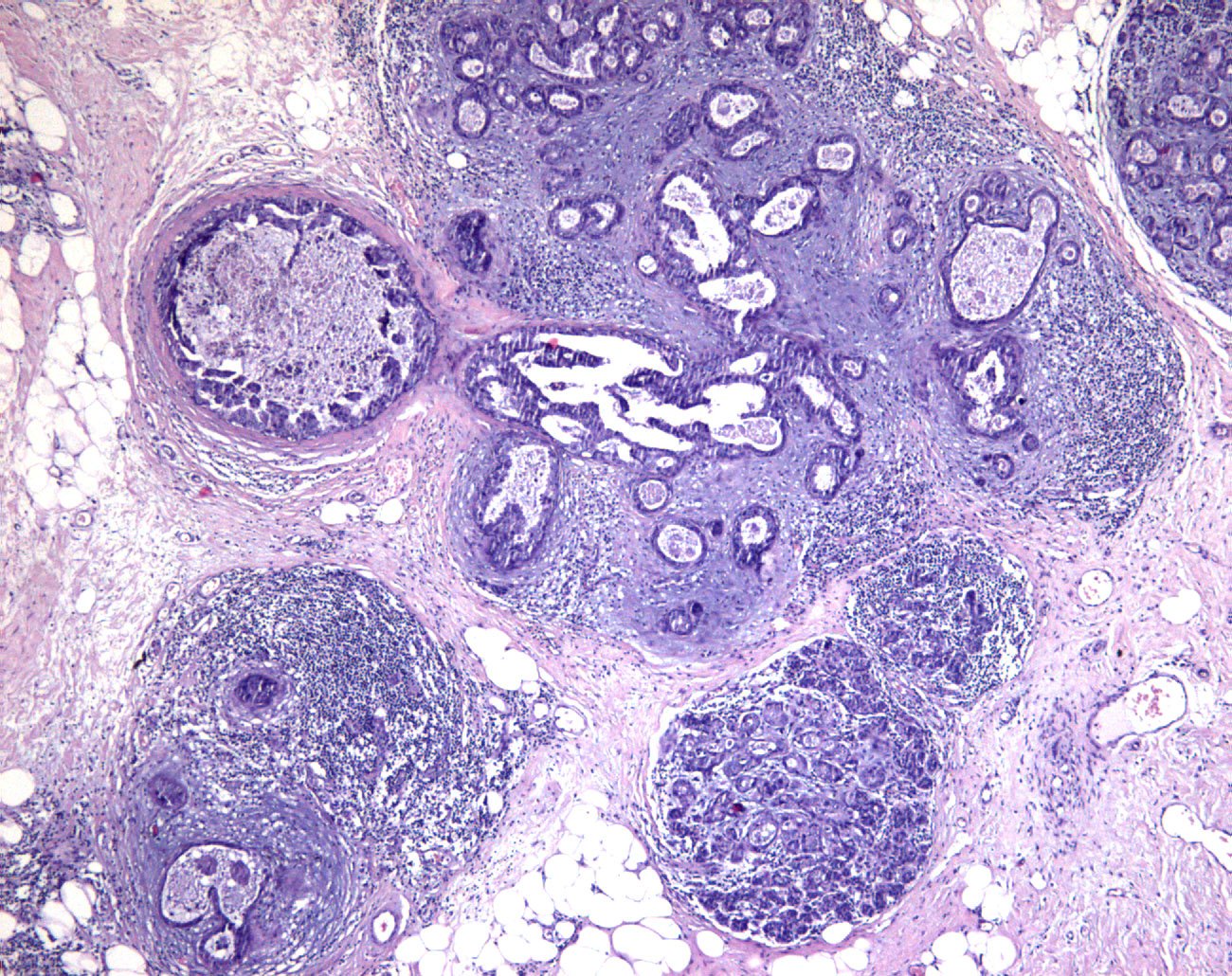
Distinction of isolated tumour cells and micrometastasis in lymph nodes of breast cancer patients according to the new Tumour Node Metastasis (TNM) definitions
Cserni, G., I. Amendoeira, S. Bianchi, E. Chmielik, J. Degaetano, D. Faverly, P. Figueiredo, M. P. Foschini, D. Grabau, J. Jacquemier, H. Kaya, J. Kulka, M. Lacerda, I. Liepniece-Karele, J. M. Penuela, C. Quinn, P. Regitnig, A. Reiner-Concin, A. Sapino, P. J. van Diest, Z. Varga, V. Vezzosi, J. Wesseling, V. Zolota, E. Zozaya and C. A. Wells (2011).
Eur J Cancer 47(6): 887-894.
http://www.ncbi.nlm.nih.gov/pubmed/21168328
Isolated tumour cells and micrometastases represent two different staging categories and are often dealt with differently when identified in sentinel lymph nodes of breast cancer patients. The reproducibility of these categories was found to be suboptimal in several studies. The new edition of the TNM (Tumour Node Metastasis) is expected to improve the reproducibility of these categories. Fifty cases of possible low-volume nodal involvement were represented by one to four digital images and were analysed by members of the European Working Group for Breast Screening Pathology (EWGBSP). The kappa value for interobserver agreement of the pN (TNM) staging categories and of the isolated tumour cells category were 0.55 and 0.56 reflecting moderate reproducibility, and the kappa of the micrometastatic category (0.62) reflected substantial reproducibility. This is an improvement over the results gained on the basis of the previous edition of the TNM. Maximal adherence to the category definitions supplemented by explanatory texts in the staging manual should result in more homogeneous nodal staging of breast cancer.